Revolutionizing Healthcare Claims with AI Agentic Automation
Healthcare organizations face massive administrative burdens from claim validation, eligibility checking, and regulatory compliance. One of the largest insurance providers partnered with myAiLabs to automate its end-to-end claims management. Using NLP-powered AI agents, myAiLabs delivered measurable transformation—54% faster claim processing, 79% first-pass accuracy, and a 24% reduction in operational costs.
🎯 The Challenge: Complexity Slowing Care
With over 50,000 claims arriving daily across multiple data formats—faxed forms, scanned PDFs, handwritten notes—manual validation was painfully slow. Multiple system dependencies, incomplete data, and inconsistent coding further delayed reimbursements. Claims staff spent hours reconciling mismatched policy information, severely impacting both efficiency and member satisfaction.
The healthcare enterprise needed a solution that could understand medical language, automate repetitive tasks, and maintain airtight regulatory compliance.
🤖 The myAiLabs Agentic Solution
myAiLabs implemented its AI Agentic Intelligent Claims Processing Platform, an orchestrated ecosystem of AI agents designed to handle every stage of claims processing with seamless collaboration and relentless precision.
Our Principal AI Agents:
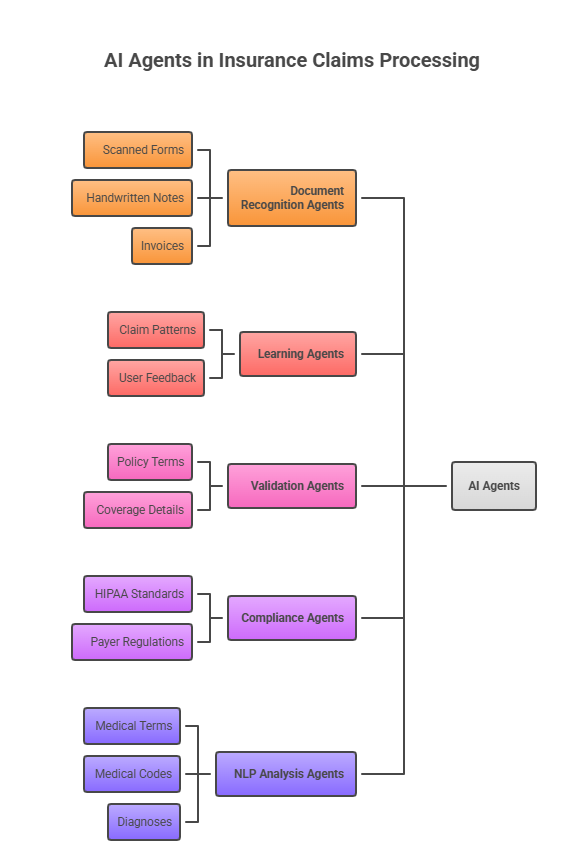
Document Recognition Agents
Digitize and categorize unstructured files, including scanned forms, handwritten notes, and invoices.
Learning Agents
Continuously refining models based on claim patterns and user feedback to improve accuracy.
Validation Agents
Match procedures against policy terms and coverage details in seconds.
Compliance Agents
Ensure every decision meet HIPAA and payer regulatory standards.
NLP Analysis Agents
Interpret medical terms, codes, and diagnoses using real-time natural language understanding.
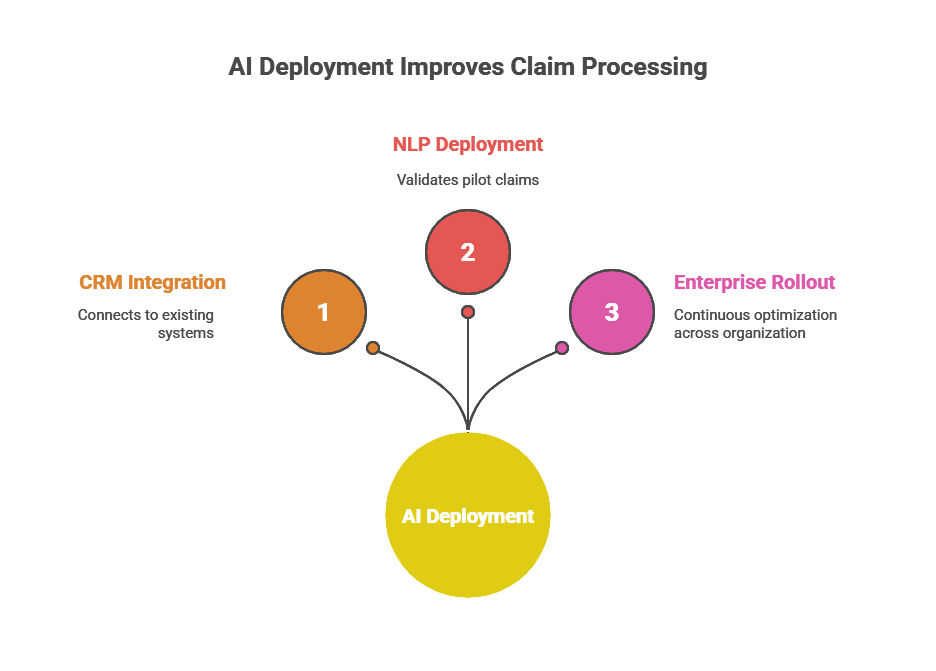
Implementation Journey
Deployment Timeline: 10 weeks total.
- Phase 1: Integration with existing CRM and EMR systems.
- Phase 2: Deployment of NLP and validation agents for pilot claims batch.
- Phase 3: Enterprise-wide rollout and continuous optimization.
Every successfully processed claim improved the AI models, creating a continuous feedback loop that steadily enhanced performance.
📈 Measurable Results
Performance Metrics:
- 54% faster claim processing time
- 79% first-pass accuracy rate
- 24% reduction in operational costs
- Handling capacity increased by 125%
Additional Benefits:
- Provider payments processed days faster
- Error-prone human validation steps nearly eliminated
- Enhanced audit readiness and compliance visibility through explainable AI
🌐 Transformation That Scales
The client now leverages the platform's AI agentic intelligence for adjacent processes—pre-authorization, utilization review, and denial management—driving further efficiency and operational agility.
Result
A self-optimizing, fully compliant, and intelligent claims ecosystem that is reshaping modern healthcare administration.
