
Healthcare organizations across the globe are under immense pressure to reduce administrative overhead while improving speed, accuracy, and compliance. One of the most complex and resource-intensive processes is claims processing—from eligibility checks and document validation to regulatory compliance and reimbursements.
To address these challenges, a leading healthcare insurance provider partnered with myAiLabs to implement an AI Agentic Intelligent Claims Processing platform, achieving dramatic improvements in efficiency, accuracy, and cost savings.
The Growing Challenge of Healthcare Claims Processing
Healthcare payers manage tens of thousands of claims every day. These claims arrive in multiple formats such as:
- Scanned PDFs
- Faxed forms
- Handwritten medical notes
- Digital and semi-structured documents
Manual processing of such high-volume, unstructured data leads to:
- Delayed claim approvals
- Inconsistent coding and eligibility errors
- Increased operational costs
- Poor provider and member experience
Claims teams often spend hours reconciling incomplete or mismatched policy information, slowing reimbursements and creating compliance risks.
The need was clear: an intelligent, automated, and compliant claims processing system capable of understanding medical language and adapting over time.
The myAiLabs Agentic Approach to Intelligent Claims Processing
myAiLabs implemented an AI Agentic Automation Platform—a collaborative ecosystem of specialized AI agents that work together to manage the complete claims lifecycle.
Instead of relying on rule-based automation, the platform uses learning, reasoning, and orchestration capabilities to continuously improve outcomes.
Core AI Agents Powering the Claims Platform
Document Recognition Agents
These agents automatically digitize, classify, and extract data from unstructured documents such as scanned forms, invoices, and handwritten notes.
NLP Analysis Agents
Using advanced natural language processing, these agents interpret medical terminology, diagnosis codes, procedures, and payer rules with high contextual accuracy.
Validation Agents
Validation agents instantly cross-check claims against policy coverage, eligibility rules, and procedure codes, eliminating manual reconciliation.
Compliance Agents
Designed to meet healthcare regulatory standards, these agents ensure every claim adheres to HIPAA and payer-specific compliance requirements.
Learning Agents Learning agents continuously refine models using historical claim patterns and feedback, improving accuracy with every processed claim.
Implementation Journey: From Integration to Optimization
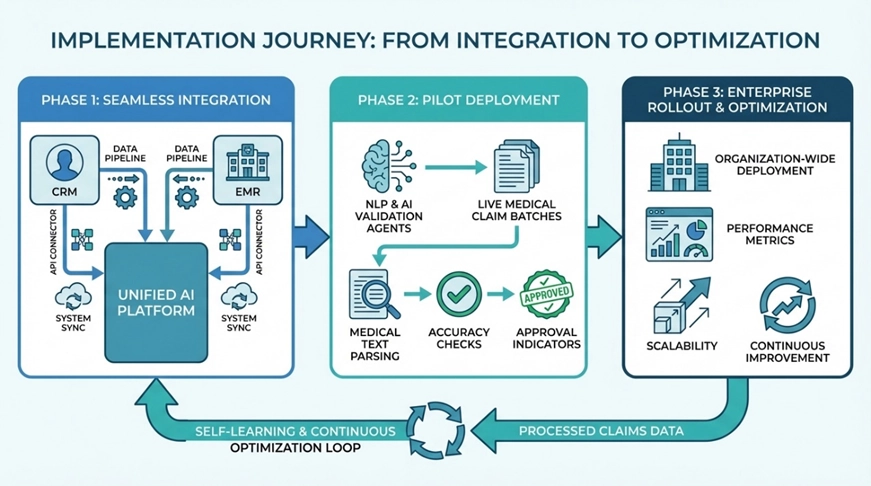
The entire platform was deployed in just 10 weeks, following a phased approach:
Phase 1: Seamless integration with existing CRM and EMR systems
Phase 2: Pilot deployment of NLP and validation agents on live claim batches
Phase 3: Enterprise-wide rollout with continuous optimization
Each processed claim fed new insights back into the system, creating a self-improving feedback loop.
Measurable Business Impact
Performance Improvements
- 54% faster claim processing time
- 79% first-pass accuracy rate
- 24% reduction in operational costs
- 125% increase in claims handling capacity
Additional Business Benefits
- Faster provider payments
- Near-elimination of manual validation errors
- Improved audit readiness with explainable AI decisions
Enhanced regulatory visibility and transparency
Scaling Beyond Claims Processing
With proven success, the healthcare organization expanded AI agentic intelligence into adjacent workflows such as:
- Pre-authorization
- Utilization review
- Denial management
This expansion unlocked new levels of operational agility while maintaining strict compliance standards.
The Result: A Smarter Healthcare Claims Ecosystem
The organization now operates a fully compliant, self-optimizing, and intelligent claims processing ecosystem. Claims move faster, accuracy is consistently high, and operational teams are freed from repetitive administrative tasks, allowing them to focus on delivering better care experiences.
Ready to Reimagine Your Healthcare Claims Operations?
Intelligent Claims Processing powered by AI agents can dramatically reduce cycle times, improve first-pass accuracy, and lower operational costs while maintaining regulatory confidence.
Transform your claims operations with myAiLabs and move from manual processing to intelligent automation.